DEB's Audiology & Hearing Care
- +91 8850 769 404
- info@debsaudiology.com
- Follow Us :
BERA Test: What It Is, Why Your Baby May Need It, and What to Expect
By DEB’s Audiology Team – May 2026 – 12 min read
Article Summary
A BERA test referral can be stressful, but it is a safe and painless way to accurately assess a child’s hearing. This guide clarifies that BERA and ABR are the same test and explains why it is essential after a failed newborn screen or for children with speech delays.
The resource outlines exactly what to expect, from prepping your baby for a “natural sleep” state to understanding the final results. By explaining how the test measures the entire auditory pathway, it provides a clear roadmap for families to secure a definitive diagnosis and plan the next steps for their child’s development
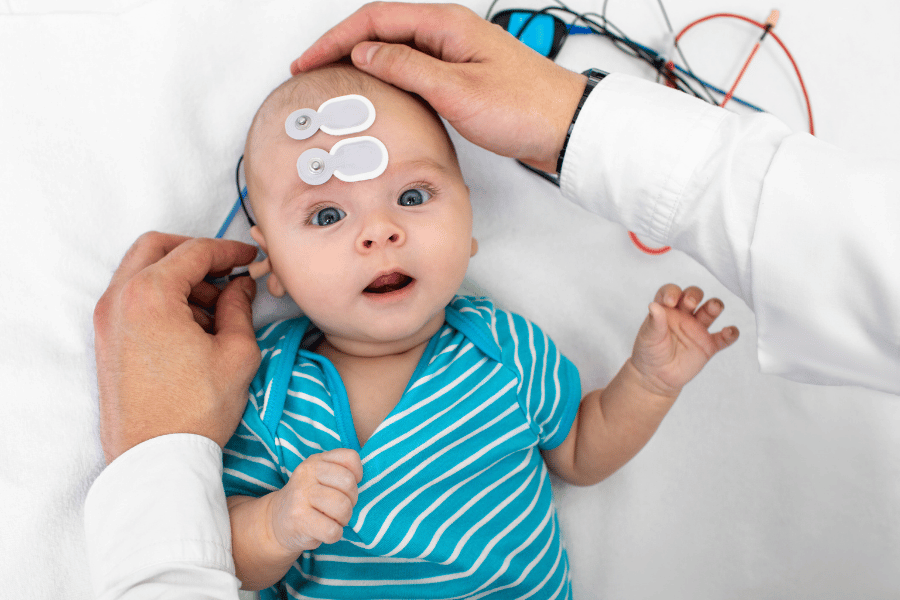
If your baby has been referred for a BERA test, you are probably worried. That is entirely normal. Being told your newborn needs further hearing investigation is frightening for any parent.
This guide will explain what the BERA test is, why it has been recommended, what happens during the test, and what the results mean – in plain language, not medical jargon. The BERA test is safe, painless, and one of the most important diagnostic tools in paediatric audiology.
BERA and ABR: The Same Test, Different Names
If you have been searching online, you may have encountered multiple names for this test: BERA, ABR, BAER, BAEP, and Auditory Brainstem Response. These are all the same test. The terminology varies by hospital, country, and medical tradition, but the procedure and the information it provides are identical.
In India, the term BERA (Brainstem Evoked Response Audiometry) is most commonly used by hospitals and paediatricians. Internationally, ABR (Auditory Brainstem Response) is the standard term. Throughout this article, we use BERA because that is the term you are most likely to have heard from your doctor – but if you see ABR elsewhere, know that it is the same investigation.
Important distinction: BERA (the diagnostic test described in this article) is not the same as AABR (Automated ABR). AABR is the automated, bedside screening version used in hospitals in the first days of life – it gives a quick pass or refer result. BERA is the full diagnostic follow-up, performed in an audiology clinic, that provides detailed threshold information about your child’s hearing.
What Does the BERA Test Actually Measure?
The BERA test measures how sound travels from your child’s ear through the auditory nerve to the brainstem. It does this by playing a series of clicking sounds through small earphones and recording the brain’s electrical response using sensors placed on the head.
The test produces a series of waveforms (labelled Wave I through Wave V) that show how the auditory signal is processed at each stage of the pathway. The audiologist analyses the timing, shape, and amplitude of these waves to determine two things:
- Hearing threshold: The softest sound level at which Wave V can still be identified. This tells us the degree of hearing loss, if any
- Pathway integrity: Whether the signal is travelling normally from the cochlea through the auditory nerve to the brainstem. Abnormal wave patterns or timing can indicate problems beyond the inner ear
Critically, the BERA test does not require the child to respond, cooperate, or be awake. The brain’s response is recorded automatically. This is why it is the gold standard for hearing assessment in infants and young children who cannot participate in standard hearing tests.
Who Needs a BERA Test?
The most common reason for a BERA test is a failed or inconclusive newborn hearing screen. But it is also used in several other clinical situations:
- Infants who failed the OAE or AABR newborn screen. A refer result on the birth screen does not confirm hearing loss – it means further investigation is needed. BERA is that investigation. The international 1-3-6 benchmark recommends completing diagnostic BERA by 3 months of age
- Children with speech or language delay. If a child is not meeting speech milestones, hearing loss must be ruled out first. BERA provides an objective assessment that does not depend on the child’s cooperation
- Children with developmental delay, autism spectrum disorder, or NICU history. These children are at higher risk of hearing loss and may not respond reliably to standard hearing tests
- Children with recurrent ear infections. To determine whether repeated infections have caused permanent hearing damage beyond the treatable conductive component
- Family history of childhood hearing loss. Genetic hearing loss may not be apparent at birth and can develop in the first months of life. BERA provides an objective baseline
- Adults with asymmetric hearing loss or suspected retro-cochlear pathology. BERA can identify auditory nerve or brainstem disorders such as acoustic neuroma, auditory neuropathy, or multiple sclerosis
BERA vs OAE: What’s the Difference?
This is one of the most common questions parents ask, and the distinction matters:
OAE (Otoacoustic Emissions) is a screening test that checks whether the cochlea (inner ear) is producing sounds in response to stimulation. It is quick, automated, and typically the first test a newborn receives. OAE tells us whether the cochlea is functioning – but it cannot assess the auditory nerve or the brainstem pathways beyond the cochlea.
BERA is a diagnostic test that examines the entire auditory pathway – from the cochlea, through the auditory nerve, to the brainstem. It provides detailed threshold information and can identify where in the pathway a problem lies.
OAE screens the cochlea. BERA confirms or rules out hearing loss and identifies where in the pathway any problem lies. A “refer” on the OAE is the start of the diagnostic process, not the conclusion
Hearing Loss, Isolation, and Dementia – Why Treatment Matters
This section is for families on the fence about whether hearing aids are “worth it” for an elderly parent.
Untreated hearing loss does more than make conversations difficult. It drives social isolation – because people who can’t hear well gradually withdraw from challenging situations. Family gatherings. Religious events. Phone calls with grandchildren. Over time, the world gets smaller.
The 2020 Lancet Commission on Dementia Prevention identified untreated hearing loss as the single largest modifiable risk factor for dementia – greater than smoking, depression, or physical inactivity. Research from Johns Hopkins found that even mild hearing loss doubles the risk of cognitive decline, and moderate loss triples it.
Treating hearing loss with hearing aids does not guarantee dementia prevention. But it addresses the largest risk factor we can do something about.
How to Approach the Conversation with Your Parent
- Lead with concern, not criticism. “I’ve noticed you seem tired after family dinners” is better than “You can’t hear anything anymore”
- Make it about connection, not the device. “I want to make sure you can enjoy conversations with the grandchildren” is more motivating than “You need hearing aids”
- Offer to go together. The first appointment feels less daunting with a family member present. At DEB’s, we encourage family to attend
- Remove the pressure. “Let’s just get a hearing test done and see what the results say – no obligation to buy anything”
Show them modern hearing aids. Many seniors are surprised by how small and discreet current devices are. A quick image search can shift perceptions
What Happens at the First Appointment
At DEB’s Audiology, a first visit for a senior parent typically includes:
- A detailed discussion about hearing concerns – with both the patient and the family member
- Ear examination to check for wax or other treatable conditions
- Comprehensive hearing assessment (pure-tone and speech audiometry)
- A clear, jargon-free explanation of results
- Discussion of options – if hearing aids are appropriate
- No pressure to decide on the same day
The entire appointment takes 60–90 minutes. Both Dr. Nabarun and Dr. Sarmistha are experienced in working with elderly patients and understand the pace and sensitivity this requires.
Helping a Parent with Hearing Loss?
Book a comprehensive hearing assessment for your parent at DEB’s Audiology. You’re welcome to attend. We’ll evaluate their hearing, explain results to both of you, and discuss options with no pressure.
Recent Post
Have A Question?
Call or WhatsApp:
+91 88507 69404
Email: info@debsaudiology.com